Hypertension - ACCP
HypertensionBy Toni L. Ripley, Pharm.D., FCCP, BCPS, AHSCP-CHC;and Anna Barbato, Pharm.D., BCPS, AHSCP-CHCReviewed by Adam Bress, Pharm.D., MS; David L. Nickerson, Pharm.D., BCPS; and Kathryn Rice, Pharm.D., BCPSLearning Objectives1.Distinguish between the recommendations for hypertension management among recent hypertension- and disease-specificguidelines.2.Justify blood pressure goals for individual patients on the basis of the primary literature and hypertension guidelines.3.Apply understanding of blood pressure results and measurement technique to a patient case.4.Design an evaluation and treatment plan for a patient presenting with hypertension.Abbreviations in This rican Academy of FamilyPhysiciansAmbulatory blood pressuremonitoringAmerican College of CardiologyAmerican College of PhysiciansAmerican Heart AssociationAutomated office blood pressureAtherosclerotic cardiovasculardiseaseCardiovascularJoint National CommitteeMineralocorticoid receptorantagonistRenin-angiotensin systemTarget organ damageTable of other common abbreviations.IntroductionHypertension OverviewBlood pressure elevations are associated with an increased risk ofcardiovascular (CV) disease in a linear fashion. Starting at a bloodpressure of 115/75 mm Hg, every increase of 20 mm Hg in systolicblood pressure (SBP) and/or increase of 10 mm Hg in diastolic bloodpressure (DBP) is associated with a doubling of the risk of death fromstroke, heart disease, or other vascular disease (Lewington 2002).Increases in SBP have the strongest link with CV disease, thoughother blood pressure components have been linked to CV disease aswell, including DBP, pulse pressure, blood pressure variability, andmean arterial blood pressure (Whelton 2018; Muntner 2015).This chapter will review the new recommendations for blood pressure management and will focus on the pharmacotherapy of hypertension. Because hypertension is largely managed with drug therapy,clinical pharmacists often participate in management, especiallywhen hypertension may be difficult to manage because of factorssuch as adverse effects or resistant hypertension.Hypertension EpidemiologyThe prevalence of hypertension in U.S. adults has continued toincrease. In 2018, the American Heart Association (AHA) heart disease and stroke statistics update reported that about 34% of U.S.adults had hypertension, using a diagnostic SBP/DBP threshold of140/90 mm Hg (Benjamin 2018). However, the American College ofCardiology and AHA (ACC/AHA) 2017 blood pressure guidelines lowered the threshold for the diagnosis of hypertension to an SBP/DBPof 130/80 mm Hg, which led to a new hypertension prevalence of 46%of U.S. adults. Despite the 12 percentage point increase in prevalencewith the lower diagnostic threshold, the 2017 ACC/AHA blood pressure guideline estimates that only an additional 2% of patients willbe recommended antihypertensive medications because the newguideline does not recommend that all patients with blood pressurePSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 77Hypertension20/12/18 10:57 am
Joint National Committee Guidelinesreadings of 130–139/80–89 mm Hg should receive drug therapy (Muntner 2018).Hypertension prevalence increases as patients age. Usingthe lower threshold as defined by the 2017 ACC/AHA guidelines, the prevalence of hypertension for patients 20–44 yearsof age is 30% in men and 19% in women. This increases to 77%for men and 75% for women 65–74 years of age (Whelton 2018).Hypertension prevalence also differs on the basis of ethnicity and sex. Overall, hypertension is more prevalent inblacks, with an estimated prevalence of 59% and 56% in blackmen and women, respectively. White, Asian, and Hispanicmen have a prevalence of 47%, 45%, and 44%, respectively,and white, Asian, and Hispanic women have an estimatedprevalence of 41%, 36%, and 42%, respectively (Whelton 2018).These numbers are based on the 2017 ACC/AHA guidelinesand are higher than previous estimates because of the lowerdiagnostic threshold for hypertension in the new guidelines.The Joint National Committee (JNC) published the first hypertension management guidelines in the 1970s. These guidelines were constructed primarily as an expert consensusrather than an evidence-based set of recommendations.Nonetheless, the JNC guidelines were the authoritative recommendations for hypertension until 2013, when the NationalHeart, Lung, and Blood Institute (NHLBI) announced the transfer of responsibility for guideline development to other organizations. At that time, the ACC and AHA accepted responsibility forleading the development of comprehensive and evidence-basedhypertension guidelines. At the same time, the NHLBI publishedthe recommendations of the JNC 8 committee.Although this was a controversial publication, the intent ofthe JNC 8 committee was to bridge the gap between JNC 7and the new ACC/AHA guidelines that were in development,given that JNC 7 was published in 2003 and many believedit to be outdated. For example, JNC 7 recommended β-blockers as an acceptable first-line therapy, whereas by 2017, mosthypertension experts considered β-blockers to be inferior toother first-line hypertension medications in the absence ofcompelling indications.The JNC 7 guidelines were a comprehensive expert consensus of the prevention, detection, evaluation, and treatment ofhigh blood pressure in adults (Chobanian 2003), whereas theJNC 8 guidelines were an evidence-based, focused set of recommendations. The JNC 8 panel chose three critical questionson which to focus its update (Box 1) and revised the processsuch that recommendations were graded on the basis of theavailable evidence, as is the contemporary guideline standard.One unique aspect of JNC 8 was the evidence included in itsreview to inform its recommendations. Only randomized controlled clinical trials were reviewed; meta-analyses, systematicreviews, and epidemiologic analyses were excluded. Although theintention to restrict review to the gold standard evidence of randomized trials is understandable, the process was criticized for notconsidering the totality of evidence for managing hypertension.Clinical Guideline UpdateIn 2017, the long-awaited ACC/AHA guidelines for the prevention,detection, evaluation, and management of high BP in adults werepublished. These are the first comprehensive, evidence-basedguidelines for hypertension in the United States.Baseline Knowledge StatementsReaders of this chapter are presumed to be familiarwith the following: Pathophysiology of hypertension. Knowledge of parenteral agents used to treathypertension. Knowledge of oral pharmacologic agents used totreat hypertension.Consequences of poor blood pressure control.Standard process of blood pressure measurement.Table of common laboratory reference valuesBox 1. Critical Questions Addressedin JNC 8Additional ReadingsThe following resources have additional backgroundinformation on this topic: Seventh Report of the Joint National Committee onPrevention, Detection, Evaluation, and Treatment ofHigh Blood Pressure: the JNC 7 report. JAMA2003;289:2560-672.2014 evidence-based guideline for the management of high blood pressure in adults: report fromthe panel members appointed to the Eighth JointNational Committee (JNC 8). JAMA2014;311:507-20.BP blood pressure.Information from: James PA, Oparil S, Carter BL, et al. 2014evidence-based guidelines for the management of high bloodpressure in adults. Report from the panel members appointedto the Eighth Joint National Committee (JNC 8). JAMA2014;311:507-20.ASCVD risk calculator.2017 ACC/AHA hypertension guidelines.PSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 8In adults with hypertension:1. Does initiating antihypertensive pharmacologic therapyat specific BP thresholds improve health outcomes?2. Does treatment with antihypertensive pharmacologictherapy to a specified BP goal improve health outcomes?3. Do various antihypertensive drugs or drug classesdiffer in comparative benefits and harms on specifichealth outcomes?8Hypertension20/12/18 10:57 am
The JNC 8 guidelines contained nine recommendationssurrounding the three critical questions. The most controversial recommendation was to relax the target blood pressurefor adults without diabetes or chronic kidney disease, age 60and older, to less than 150/90 mm Hg. In fact, a group withinthe JNC 8 committee separately published a “minority view”supporting the continued goal of less than 140/90 mm Hg foradults 60 and older (Wright 2014). These authors cited concerns about the adverse effects on public health if blood pressure goals were relaxed in older patients because older ageis a risk factor for CV disease. Although no randomized controlled trials supported treating patients 60 and older to lessthan 140/90 mm Hg, they contended that there were also nodata at the time to support the higher blood pressure target.However, some guidelines remain that were not developedin collaboration with the ACC or AHA that continue to supportclinical practice. The American College of Physicians (ACP)and the American Academy of Family Physicians (AAFP) published recommendations for managing hypertension in adultpatients 60 and older in early 2017, before release of the 2017ACC/AHA guidelines (Qaseem 2017). After publication ofACC/AHA guidelines, the ACP and AAFP published a statement that they would not be endorsing the ACC/AHA hypertension recommendations (Crawford 2017). Hence, the ACP/AAFP 2017 guidelines should be considered a current andactive set of recommendations.Finally, the role of the JNC 8 panel recommendations remainsless clear. Some groups such as ACP and AAFP have endorsedthe JNC 8 recommendations. However, JNC 8 is not a comprehensive guideline and leaves many questions unanswered.Table 1 presents highlights from the guideline recommendations.BP blood pressure; TIA transient ischemic attack.Other Hypertension GuidelinesThe delay in comprehensive U.S. guidelines led to a surge inblood pressure recommendations from several groups. Manyof these guidelines were focused on subgroups, such as thosewith heart failure, coronary artery disease, or stroke. Guidelines such as these were developed by the ACC; therefore, itis reasonable to consider that the goals recommended by the2017 ACC/AHA guidelines supersede former blood pressurerecommendations by past ACC-endorsed guidelines.2017 ACC/AHA Recommendations for ManagingHypertension in AdultsThe 2017 ACC and AHA updated guidelines were endorsed bymany other organizations. The guidelines are extensive, andseveral recommendations are new and worthy of discussion.Table 1. Comparison of BP Target RecommendationsBP CategoriesaSBP(mm Hg)DBP(mm Hg)Normal 120 80Prehypertension120–13980–89Stage 1 hypertension140–15990–99Stage 2 hypertension 160 100BP TargetsJNC 7, 2003 140/90 mm Hg 130/80 mm Hg for those with diabetesor chronic kidney diseaseJNC 8, 2014 150/90 mm Hg for patients 60 140/90 mm Hg for patients 60, diabetes,and chronic kidney diseaseWas not a comprehensive set of recommendations, and didnot discuss hypertension diagnostic thresholdsACP/AAFP, 2017 150/90 mm Hg for patients 60 140/90 mm Hg for patients at higher CVrisk, or with a history of stroke or TIAWas not a comprehensive set of recommendations and didnot discuss hypertension diagnostic thresholdsDid not address recommendations in patients 60ACC/AHA, 2017 130/80 mm HgNormalElevatedStage 1 hypertensionbStage 2 hypertensiona 120 80120–129 80130–13980–89 140 90Patients with SBP and DBP in two different categories should be classified in the higher category.Antihypertensive medication should be initiated in stage 1 hypertension only in patients with clinical CV disease, a 10-year risk ofASCVD of 10% or higher, diabetes mellitus, or chronic kidney disease.BP blood pressure; TIA transient ischemic attack.bPSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 99Hypertension20/12/18 10:57 am
Treatment GoalsNew Diagnostic Criteria and StagingThe 2017 guidelines lowered the threshold for the diagnosisof hypertension to 130/80 mm Hg from the 140/90 mm Hgstandard of the past several decades. The JNC 7 guidelinescategorized patients with a blood pressure of 130–139/80–89 mm Hg as “pre” hypertensive on the basis of cohort datashowing a gradient of increased CV risk as SBP crossed thethreshold of 120 mm Hg. The lower threshold for the diagnosis of hypertension increased the prevalence of hypertension,as previously discussed.The 2017 guidelines also updated the blood pressure categories (see Table 1) and highlighted the blood pressure measurement technique (discussed below).Epidemiologic evidence has shown that the risk of vasculardeath increases as blood pressure increases above 115/75mm Hg (Lewington 2002).Blood pressure goals have been intensely debated since2013, when the JNC 8 recommendations became available. Whereas the thet JNC 8 recommendation to relax theSBP goals from less than 140 mm Hg to less than 150 mmHg in patients older than 60 without diabetes or kidney disease was met with criticism, the 2017 ACC/AHA hypertension guidelines now call for stricter blood pressure control.A review of clinical trials that have tried to tackle this challenging question regarding optimal blood pressure targetsfollows. Of importance, several well-conducted meta-analyses have further explored this issue (Bundy 2017; Reboussin2017). A comprehensive review of this complicated questionis beyond the scope of this chapter.Risk AssessmentThe 2017 ACC/AHA guidelines recommend incorporating CVrisk estimates with blood pressure levels to determine whento initiate antihypertensives. The guidelines suggest initiating medication in those at high CV risk when SBP is 130 mmHg or greater or DBP is 80 mm Hg or greater. In those at lowerCV risk, they suggest initiating antihypertensives when SBPis 140 mm Hg or greater or DBP is 90 mm Hg or greater (Whelton 2018).High CV risk is defined as a history of clinical CV diseaseor an estimated 10-year atherosclerotic CV disease (ASCVD)risk of 10% or higher according to the pooled cohort equations. Clinical CV disease is defined as coronary artery disease, heart failure, or stroke.The inclusion of risk estimation in determining whento initiate antihypertensives comes, in part, from SPRINT,which included CV risk assessment as part of the inclusion criteria. Using the 10-year Framingham risk score, theSPRINT investigators set the threshold for high CV risk at15%, which has been estimated to be similar to a 10-yearASCVD risk of 6–7% according to the pooled cohort equations (Whelton 2018).Use of the pooled cohort equations has been controversial,given that their role for estimating the risk of initiating antihypertensives has not been formally evaluated in a clinical trial.Conversely, the pooled cohort equations have become morecommon in clinical practice and are integrated into someelectronic medical records for efficient risk assessment.The pooled cohort equations are also used to determine theappropriate drug therapy for dyslipidemia and have played arole as the contemporary CV risk estimator, in place of Framingham, since 2014.Although evidence to evaluate the pooled cohort equations in hypertension is beginning to surface, their use andthe thresholds to consider for various risk levels continue tobe debated. Regardless of the method used to assess CV risk,clinicians must be aware that CV risk should be considered inhypertension management, given that the benefits of treatinghypertension are greatest in those with the highest CV risk(Muntner 2017).PSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 10SPRINTThe Systolic Blood Pressure Intervention Trial (SPRINT) was asentinel clinical trial that compared CV outcomes in patientsdiseasewith increased CV risk who were randomized to anintensive blood pressure goal of less than 120 mm Hg or astandard blood pressure goal of less than 140 mm Hg (Wright2015). This trial has affected hypertension management andclinical guidelines more than any other trial since the landmark Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT).In the SPRINT study, more than 9000 patients were randomized. ).)To be included, patients had to be 50 or older andhave an increased CV risk, defined as clinical or subclinicalCV disease, chronic kidney disease, or a 10-year CV risk of15% or more on the basis of the Framingham risk score, or be75 or older. On average, patients were 68 years of age with abaseline blood pressure of 140/78 mm Hg, about 28% were 75or older, 17% had clinical CV disease, and the average 10-yearCV risk score was 25%.Diastolic BP was not a criterion for inclusion in SPRINT. Eligibility was based on a combination of SBP and the numberof antihypertensive medications being taken at enrollment.Patients with an SBP of 130–180 mm Hg and taking no morethan four antihypertensives were included.Patients with a history of stroke or diabetes, symptomaticheart failure or heart failure with an ejection fraction less than35%, severely elevated blood pressure (defined as SBP greaterthan 180 mm Hg), orthostasis (defined as an SBP decrease toless than 110 mm Hg after 1 minute of standing) and nursinghome patients were excluded from the SPRINT trial.Exclusion of patients with diabetes was based on the ACCORDtrial, which was ongoing at the time SPRINT was designed, withthe thought that intensive blood pressure control in patientswith diabetes was already being adequately evaluated.Of note, 14,692 patients were screened for enrollment, and5331 were ineligible to participate. Forty-three percent of the10Hypertension20/12/18 10:57 am
excluded patients were excluded because they took too manymedications or had an SBP out of the range noted previously.The primary composite outcome was myocardial infarction (MI), non-MI acute coronary syndromes, stroke, heartfailure, or death from CV causes.The trial was terminated early, after 3.26 years of follow-up,because of the significant benefits in those randomized to theintensive blood pressure arm. Patients in the intensive groupachieved an average SBP of 121.5 mm Hg compared with 134.6mm Hg in patients in the standard care group, taking an average of 2.8 and 1.8 antihypertensive medications, respectively.The intensive group had a 25% relative risk reduction forthe primary composite end point compared with the standardcare group (HR 0.75; 95% CI, 0.64–0.89; p 0.001). The resultswere largely driven by a reduction in heart failure in the intensive group (HR 0.62; 95% CI, 0.45–0.84; p 0.002). No differences occurred between the groups in MI, acute coronarysyndrome, or stroke.Overall serious adverse events were similar between thegroups, but the intensive group had more hypotension, syncope, electrolyte abnormalities, and acute kidney injury thanthe standard care group. The standard care group had moreasymptomatic orthostasis (18.3% vs. 16.6%, p 0.01).Blood pressure measurement in SPRINT differed from thestandard of most clinical practices. Blood pressure in SPRINTwas assessed using an automated device that measuredblood pressure after the patient rested for 5 minutes, whichthen provided the average of three blood pressure measurements. Blood pressure assessed using this method is around10 mm Hg lower than the measurements used in most officesettings. Discussion of blood pressure measurement technique will be provided in another section.The conclusion from SPRINT is that intensive blood pressure reduction is more effective than standard blood pressurereduction at reducing CV events and all-cause mortality inpatients without diabetes or stroke who are at risk of CV disease. However, the measurement technique used in SPRINTmay limit extrapolation of the findings to settings that do notuse similar automated blood pressure measurement devices.or CV risk factors. The primary outcome was the first occurrence of a CV event, defined as a composite of nonfatal MI,nonfatal stroke, or CV death.On average, patients were 62 years of age and had a baseline blood pressure of 139/76 mm Hg; 33.7% had CV disease.Patients were followed for an average of 5 years.Patients in the intensive arm achieved a blood pressure of119.3/64.4 mm Hg and patients in the standard arm, 133.5/70.5mm Hg. Despite the blood pressure difference, the primary composite outcome was similar between the intensive and standard blood pressure treatment groups (1.87%/year vs. 2.09%/year; HR 0.88; 95% CI, 0.73–1.06; p 0.20). However, intensiveblood pressure reduction did reduce the rate of stroke, one ofthe prespecified secondary outcomes, compared with standard treatment (0.32%/year for intensive vs. 0.53%/year forstandard treatment; HR 0.59; 95% CI, 0.39–0.89; p 0.01).Patients in the intensive blood pressure treatment arm hadmore hypotension, syncope, bradycardia, increases in serumcreatinine, and hypokalemia than did patients in the standardtreatment group.The conclusion from the ACCORD BP trial is that intensiveblood pressure management in patients with type 2 diabetesdoes not improve CV end points, despite improved blood pressure values.HYVET StudyThe Hypertension in the Very Elderly Trial (HYVET) was oneof the first large-scale clinical trials to establish the benefitof lowering blood pressure in patients 80 and older (Beckett2008). The HYVET trial adds to our understanding of bloodpressure targets by evaluating blood pressure control in olderpatients at high risk of CV events and adverse drug events.HYVET was a non–U.S.-based study that evaluated theoccurrence of fatal or nonfatal stroke in 3845 adults with abaseline SBP of 160 mm Hg or greater taking indapamide 1.5mg daily or placebo. Perindopril 2 or 4 mg daily or placebowas added to the intervention or placebo groups, respectively, if needed, to target a goal blood pressure of less than150/80 mm Hg.Patients were, on average, 84 years of age with a baselineblood pressure of 173/91 mm Hg. Median follow-up was 1.8years. Blood pressure fell in both groups. After 2 years, themean seated blood pressure reduction in the placebo groupwas 14.5 18.5/6.8 10.5 mm Hg and was 29.5 15.4/12.9 9.5 mm Hg in the intervention group.There was a nonsignificant reduction in the primary endpoint with active treatment (p 0.06). However, there was a39% reduction in death from stroke (p 0.046), a 21% reduction in all-cause death (p 0.02), a 74% reduction in heart failure (p 0.001), and a 34% reduction in the occurrence of anyCV event (p 0.001).The conclusion from HYVET supports targeting a bloodpressure goal of less than 150/80 mm Hg for patients withhypertension who are older than 80.ACCORD BP StudyAnother important clinical trial that has influenced contemporary hypertension management is the Action to ControlCV Risk in Diabetes BP (ACCORD BP) trial (Cushman 2010).In ACCORD BP, 10,521 patients were randomized to intensiveor standard glycemic control. Patients were then further randomized in a 2 x 2 factorial design to intensive versus standard care of either blood pressure or lipids. The results of theblood pressure arm, in which 4733 patients were randomized,will be discussed here.Patients in ACCORD BP had uncontrolled type 2 diabetesand an SBP of 130–180 mm Hg on three or fewer antihypertensives. Included patients were age 40–54 with CV disease,or age 55 and older with subclinical CV disease, albuminuria,PSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 1111Hypertension20/12/18 10:57 am
SPRINT Study – Adults 75 and OlderSubanalysisIndividual characteristics should be considered whenestimating the risk of lowering DBP. For example, in olderpatients, arterial stiffness leads to elevated SBP and lowerDBP. However, lowering DBP to less than 65 or 70 mm Hg inthis specific group may increase vascular risk, and prudenceis warranted (de Boer 2017).Evaluation of the adults 75 and older enrolled in the SPRINTtrial was a prespecified analysis. Patients in this subanalysiswere 80 years of age on average and had a blood pressure of142/71 mm Hg (Williamson 2016).Thirty-one percent of patients were classified as frail,according to a 37-item index. The average 10-year risk of CVdisease was similar to that in the whole SPRINT cohort andwas 24% and 25% in the intensive and standard care groups,respectively.During follow-up, SBP was 123 mm Hg in the intensive armand 135 mm Hg in the standard care arm.The primary outcome was 34% lower in the intensive armthan in the standard care group (HR 0.66; 95% CI, 0.51–0.85).Similar to the main study results, improvement in this cohortwas primarily driven by a reduction in heart failure.The most common question in treating older patients to amore intensive blood pressure goal appears to be their tolerability of the lower blood pressure, especially frail patients, andthis analysis sought to address that question.Patients who were classified as “less fit” had a reductionin the primary composite outcome with intensive blood pressure reduction compared with standard reduction (HF 0.63;95% CI, 0.43–0.91; p 0.01). Patients who were “less fit” or“frail” also had less all-cause mortality with intensive treatment, whereas patients who were classified as “fit” had nobenefit with intensive blood pressure reduction. No difference occurred in adverse outcomes with intensive bloodpressure treatment using markers of frailty.Overall, this subanalysis helps inform hypertension management in older patients and supports a more intensivestrategy than was suggested with the recommendations fromthe panel appointed to the JNC 8 committee.Blood Pressure MeasurementThe 2017 ACC/AHA guidelines place more emphasis onproper blood pressure measurement than do previous guidelines. The impetus for this comes from the recognition thatblood pressure measurement is error prone and there ispotential for harm if a provider titrates medications to thelower blood pressure target recommended by the guidelines using a falsely elevated blood pressure measurement(Whelton 2018).Proper Measurement TechniqueStandard techniques for blood pressure measurement arewell established and can be done with manual auscultationor with an automated oscillometric device. Interest in usingautomated office blood pressure (AOBP) devices has continued to grow, given the belief that some measurement errors(e.g., auscultatory errors) can be eliminated. Furthermore,AOBP devices can be programmed to minimize the whitecoat effect by delaying blood pressure measurement suchthat the health care professional can leave the room and thepatient can be resting for a prescribed period (typically 1–5minutes) before measurement. The AOBP devices can alsoprovide an average of three readings.Given that there are different methods of measuring bloodpressure, different blood pressure results should be expected,depending on the procedure. Providers involved with managing hypertension should be familiar with the differences andshould consider these during clinical decision-making. Manual office blood pressure measurements average about 10mm Hg higher than measurements from daytime ambulatoryblood pressure monitoring (ABPM) or AOBP, whereas ABPMand AOBP usually provide similar results (Sica 2016).Of note, AOBP was used in SPRINT. Because the meanSBP achieved with intensive treatment in SPRINT was 121.4mm Hg, the 2017 ACC/AHA guidelines factored in that manyoffices are not using AOBP and recommended an SBP goal ofless than 130 mm Hg, rather than 120 mm Hg.It is vital to recognize the potential sources of error duringblood pressure measurement and how the error could affectthe blood pressure reading. Using AOBP does not removethe potential for all errors. Indeed, attention still needs to begiven to proper procedure, and patients should be instructedto maintain the correct body position and avoid talking duringmeasurement.Box 2 provides examples of factors that can cause inaccurate blood pressure readings and the direction of effect onSBP and DBP.DBP ConsiderationsAnother area of debate within hypertension management isthe threshold to which DBP can safely be lowered while targeting the lower SBP goals recommended in the 2017 ACC/AHA guidelines.The diastolic J- or U-curve phenomenon suggests that CVand stroke risk increase as DBP is reduced. The rationale forincreased risk is that most coronary and cerebral blood flowoccurs during diastole. Therefore, excessively low DBP couldcause ischemia.However, evidence is mixed about this phenomenon. Apost hoc analysis of SPRINT found a U-curve associationfor baseline DBP, but the benefit of intensely lowering SBPwas not influenced by the baseline DBP. Other nonrandomized analyses show no increased risk when DBP is loweredto achieve SBP goals. Data from observational studies andsecondary analyses suggest that a combination of low DBPand wide pulse pressure is associated with increased vascular events (Ahmed 2018).PSAP 2019 BOOK 1 Cardiology01 1 Ripley.indd 1212Hypertension20/12/18 10:57 am
Box 2. Selected Causes of BPMeasurement ErrorsBox 3. Instructions for Home BPMeasurementFactors that can falsely increase SBP and DBP: Bladder distension Cuff too small Insufficient rest period Talking during measurementFactors that can falsely decrease SBP and DBP: Cuff too large Factors that have mixed errors on SBP and DBPmeasurements: Deflating the cuff too quickly Standing or supine position rather than sitting position White-coat effectStep 1: Obtain an appropriate home BP measurement device. Choose a fully automated device (avoid auscultatoryhome devices). Choose an arm device (brachial BP). Use wrist monitorsonly for patients whose arm circumference preventsproper fitting of a brachial measurement device. Choose validated devices, if possible. Ensure correct cuff size.Step 2: Prepare for BP measurement. Empty bladder; refrain from drinking caffeine orsmoking 30 min before measurement. Rest at least 5 min before BP measurement. Sit with back supported and feet flat on the floor(legs
The JNC 7 guidelines were a comprehensive expert consen - sus of the prevention, detection, evaluation, and treatment of high blood pressure in adults (Chobanian 2003), whereas the JNC 8 guidelines were an evidence-based, focused set of rec-ommendations. The JNC 8 panel chose three critical questions
from the American College of Chest Physicians (ACCP) (Geerts 2004). National guidelines are also available, such as those published by the Scot-tish Intercollegiate Guidelines Net-work (SIGN 2003). The first ACCP recommendations were published in 1986 (ACCP/NHLBI 1986). Since then,the ACCP
Call an ACCP customer service rep-resentative at (913) 492-3311, 8 a.m. 5 p.m. (Central Time) Monday through Friday. 3. ACCP Ambulatory Care Pharmacist's . NEW ACCP PUBLICATIONS. The second edition of Clinical Pharmacy in the United States: Transformation of a Profession
Inclusion Plan ACCP is dedicated to creating and sustaining a culture of diversity, equity, and inclusion (DEI). A commitment to embrace diversity and inclusion is an ACCP core value. Strategic direction 1.5 of the 2020 ACCP Strategic Plan states that the College will employ practices that embrace DEI to fully achieve its mission.1 This priority
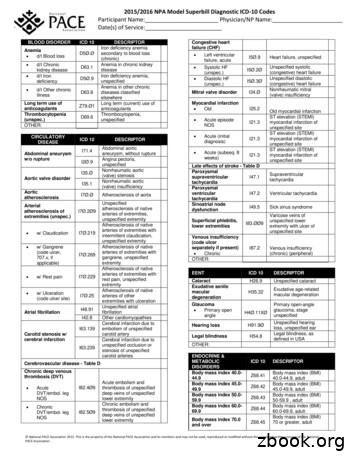
WHO ICD-11 MMS United States ICD-10-CM BA00 Essential hypertension BA00.0 Combined diastolic and systolic hypertension BA00.1 Isolated diastolic hypertension BA00.2 Isolated systolic hypertension BA00.Y Other specified essential hypertension BA00.Z Essential hypertension, unspecified Matching terms:
ICD 10 Table A- HYPERTENSION Hypertension: ICD 10 DESCRIPTOR Benign essential hypertension hypertension I1Ø Essential (primary) Essential hypertension hypertension I1Ø Essential (primary) Hypertensive heart disease:(unspecified) ICD 10
Symposium on pulmonary hypertension, pulmonary hypertension is defined as mPAP 20 mm Hg and its subgroup Pulmonary arterial hypertension (PAH) is defined as mPAP 20 mm Hg, PCWP 15 mm Hg and PVR 3 Woods Units. Table 1 : Haemodynamic definitions of pulmonary hypertension, 6th world symposium on pulmonary hypertension, Nice, France.
HYPERTENSION BELIEFS OF BARROUALLIE, ST VINCENT AND THE GRENADINES 4 4. To determine the relationship between hypertension knowledge and hypertension beliefs. Research Question 1. What are the socio- economic demographic characteristics, hypertension knowledge and hypertension beliefs among the study participants? 2.
Hypertension – Code to 401 – Only use 401.0 Malignant, or 401.1 Benign, if documentation supports – In ICD-10-CM –only one Essential (primary) Hypertension code I10 –Essential Hypertension – Includes hypertension (arterial) (benign) (essential) (malignant) (primary) (systemic); high blood pressure Hypertension with Heart .